Clinical and Equity Implications of Braidwood v. Becerra
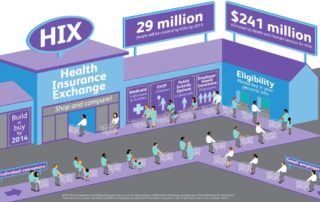
Clinical and Equity Implications of Braidwood v. Becerra AFFORDABLE CARE ACT PREVENTIVE SERVICES PROVISION Preventive services can help people avoid acute illness, identify and treat chronic conditions, prevent cancer or lead to earlier detection, and [...]